February 03, 2026
4 min read
Key takeaways:
- An estimated 37.9% of cancer cases worldwide in 2022 could be attributed to modifiable risk factors.
- The impact of these factors varies by region and sex, suggesting tailored prevention strategies are needed.
Approximately four in 10 cancer cases worldwide may be preventable, according to a new report.
An estimated 7.1 million of the 18.7 million global cancer diagnoses in 2022 — equating to 37.9% — could be attributed to modifiable risk factors, an analysis by International Agency for Research on Cancer (IARC) and WHO showed.

The impact of these risk factors varies greatly by region, and data also revealed stark differences between men and women.

Isabelle Soerjomataram
“These comparisons demonstrate why a one-size-fits-all prevention strategy is not sufficient,” Isabelle Soerjomataram, MD, PhD, a medical epidemiologist and deputy head of IARC’s cancer surveillance branch, said during a press conference. “Each country and region needs to adapt global and regional strategies and develop prevention priorities that are aligned with their specific cancer burden profile.”
Publication of the report in Nature Medicine coincides with World Cancer Day on Feb. 4. The annual observance is designed to educate the public about the importance of early detection and treatment, encourage elected representatives to commit resources to reduce cancer mortality, and increase awareness that lifestyle behaviors have a considerable effect on cancer risk.
The IARC/WHO research team aimed to conduct a comprehensive global analysis of the cancer burden attributable to 30 modifiable risk factors. These included behavioral and environmental factors, occupational exposures and infectious agents.
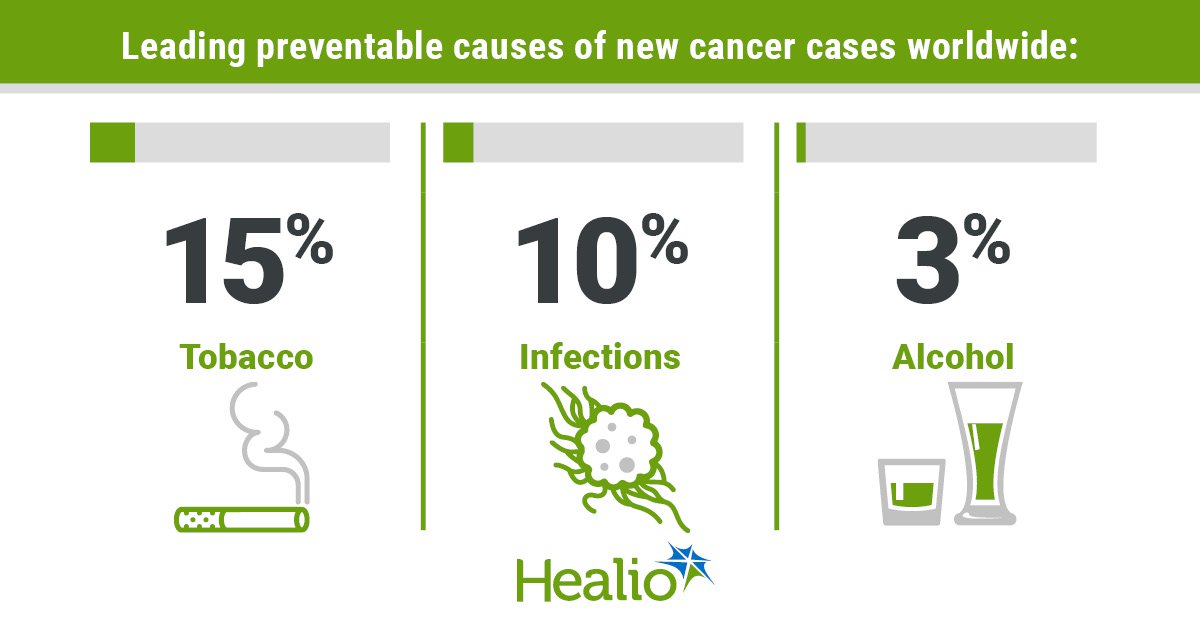
Their analysis identified tobacco as the leading preventable cause of cancer worldwide, accounting for 15% of cases in 2022. Infections ranked second, accounting for 10% of cases. Alcohol consumption ranked third, accounting for 3%.
Three cancer types accounted for close to half of preventable cancer cases, with smoking and air pollution driving lung cancer incidence, Helicobacter pylori infection primarily responsible for stomach cancer, and HPV causing most cervical cancers.
Among men, tobacco is the leading preventable cause worldwide, accounting for 45.4% of cancers and ranking first in 126 of the 185 countries evaluated. Among women, infection is the leading preventable cause worldwide, accounting for 29.7% of cancer cases and ranking first in 141 of the 185 countries evaluated.
“These striking differences reflect distinct epidemiological factors, as well as cultural and social norms, and underscore why tailored sex-responsive prevention strategies are essential to reduce the burden of cancer,” Soerjomataram said.
The impact of modifiable risk factors also varies by region.
For example, they account for a higher proportion of cancers among men than women in Eastern Asia (55.5% vs. 29.2%), Central/Eastern Europe (46.1% vs. 30.5%) and Western Europe (36.9% vs. 30.7%), but they account for a higher proportion of cancers among women in Southern Africa (43.9% vs. 33.9%) and Central America (29.4% vs. 22.1%).
Modifiable risk factors account for a comparable percentage of cancers among both men and women in North America (36.2% vs. 35.9%).
“Even in regions with lower proportions, the number of actual cancer cases that can be prevented remains substantial,” Soerjomataram said. “Prevention strategies are universally relevant. This information is crucial for governments, health systems and individuals, as it highlights where prevention reforms could have the greatest impact.”
The impact of — and outcomes after — a cancer diagnosis differs between and within countries, according to Andre Ilbawi, MD, team leader for cancer control at WHO.
“For a privileged few, access and innovation are driving survival rates beyond 70%,” Ilbawi said during the press conference. “But for far too many, cancer remains a death sentence, often compounded by devastating social and financial hardships.
“Today, we are here to celebrate good news founded on strong science: Many cancers are preventable,” he added. “Tobacco, alcohol, air pollution, unhealthy diets, physical inactivity, and infections such as HPV and hepatitis continue to drive avoidable illness and death. These risk factors place a massive strain on communities and health systems through many other diseases beyond cancer. Investing in cancer prevention, therefore, delivers wide-ranging health, societal and economic benefits.”
Declines in lung cancer incidence in the United States and United Kingdom due to reductions in tobacco use, as well as dramatic decreases in cervical cancer incidence due to screening and HPV vaccination, demonstrate that policy and public health initiatives are effective, Ilbawi said.
“The principle that we can get [the percentage of cancers attributable to modifiable risk factors] to zero isn’t a dream,” he said. “Prevention must be communicated carefully, focusing on risk reduction and not blame. It should emphasize policy and structural solutions, acknowledge uncertainty and respect the dignity of people living with cancer. Guilt and blame … harm mental health, delay care and reduce quality of life.”
In conjunction with World Cancer Day and the release of the WHO/IARC report, Healio provides the following updates on research into how modifiable risk factors such as alcohol consumption, smoking, HPV vaccination and obesity contribute to cancer risk or mortality.
1. The percentage of cancer deaths likely attributable to alcohol consumption increased by nearly 50% from 1990 to 2021. Read more.
2. Heavy alcohol intake throughout adulthood and higher lifetime alcohol consumption may significantly increase risk for colorectal cancer. Read more.
3. Even low alcohol consumption — as little as one drink per day — could contribute to thousands of breast, colorectal, oral and pharyngeal cancer diagnoses. Read more.
4. Despite increasing scientific evidence and warnings from public health advocates, nearly two-thirds of U.S. adults do not believe or do not know that drinking alcohol increases cancer risk. Read more.
5. Declines in cigarette smoking over the past several decades prevented an estimated 3.8 million lung cancer deaths, accounting for more than half of the estimated decline in overall cancer mortality between 1970 and 2022. Read more.
6. Quitting smoking soon after a cancer diagnosis can prolong survival. Individuals who quit smoking within 6 months of a cancer care appointment exhibited half the risk for all-cause mortality as those who continued to smoke. Read more.
7. Despite the benefits of smoking cessation, pain may influence cancer survivors’ decisions to use tobacco or cannabis. Read more.
8. More than 70% of U.S. adults may not know HPV causes oral cancer or other noncervical cancer malignancies. Read more.
9. Obesity-related cancer deaths increased more than threefold between 1999 and 2020. Read more.
10. GLP-1 receptor agonists may reduce cancer risk among people with obesity or overweight. Read more.
11. Nonsmokers diagnosed with obesity-related cancers had lower risk for death if they adhered to American Cancer Society nutrition and physical activity guidelines for cancer survivors. Read more.
<












Leave a Reply