April 23, 2026
3 min read
Key takeaways:
- Short sleep may be associated with reduced risk for both breast and lung cancer.
- Individuals who did not sleep 7 to 9 hours per day had significantly increased risk for head and neck cancer.
Sleep duration may have a significant impact on cancer risk.
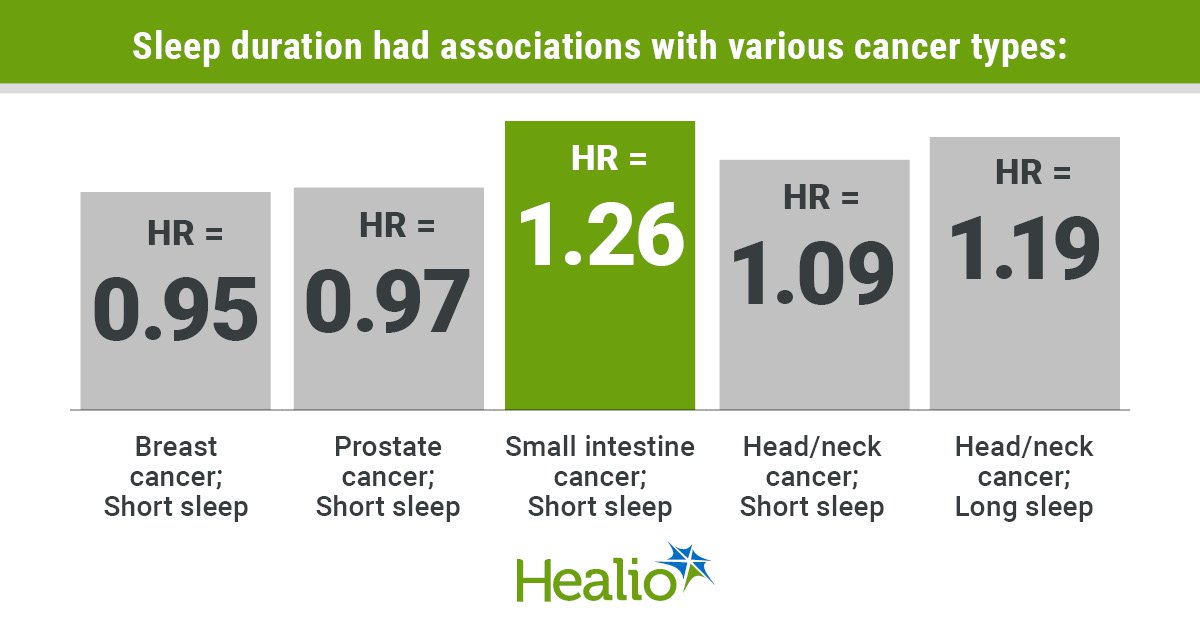
Data presented at American Association for Cancer Research Annual Meeting showed individuals who slept less than 7 to 8 hours per night had slightly lower risk for overall cancer development, and particularly for breast, lung, and skin cancers.

Data derived from Zhong C, et al. Abstract 5047. Presented at: American Association for Cancer Research Annual Meeting; April 17-22, 2026; San Diego.
However, they also had a 22% increased risk for cancer of the small intestine and 14% increased risk of acute myeloid leukemia.
Head and neck cancer risk significantly increased among individuals who had short sleep, duration, too.

Charlie Zhong
The findings highlight the “complex” association between sleep and cancer, Charlie Zhong, PhD, MPH, principal scientist in epidemiology research at American Cancer Society, and colleagues wrote.
“Ask your patients about their sleep habits,” Zhong told Healio.
Poor sleep common
Poor sleep health affects approximately a third of adults in the U.S., according to study background.
They may sleep too little, too much, or have poor quality of sleep. National Sleep Foundation recommends 7 to 9 hours of sleep per night for adults.
Prior research has shown that poor sleep health is associated with increased cardiovascular disease, morbidity and mortality, as well as with certain malignancies, including breast, colon and lung cancers.
“Cancer is sometimes a misnomer,” Zhong said. “It’s hundreds, if not thousands, of different diseases. Some behaviors are protective for one cancer, but increase risk for another. This makes it important to have large studies where we can look at individual cancers.”
Zhong and colleagues conducted a pooled meta-analysis of seven prospective cohorts to evaluate the impact sleep has on cancer development.
The investigation included 918,100 individuals (median age, 58 years; range, 34-99; 65% women).
The association between sleep duration and quality, and cancer incidence, both overall and for 29 specific types, served as the primary endpoint.
Researchers categorized short sleep as less than 7 hours per day, long sleep as more than 9 hours, and restless sleep and trouble sleep as those reporting those issues more than once per week.
Different risks for different cancers
Individuals who reported short sleep had a significantly lower risk for overall cancers (HR = 0.98; 95% CI, 0.97-0.99), breast cancer (HR = 0.97; 95% CI, 0.94-1.00), skin (HR = 0.94; 95% CI, 0.88-1.00) and lung cancer (HR = 0.97; 95% CI, 0.94-1.00).
“When it comes to breast, prostate, and some of the more hormone-driven cancers, there is some evidence that short sleep might have a protective association,” Zhong said. “Generally, the less that you’re exposed to estrogen, the less risk you have of getting breast cancer. It seems short sleep may have some effect in disrupting your hormonal balance.”
Conversely, short sleep significantly increased the risk for cancers of the small intestine (HR = 1.22; 95% CI, 1.02-1.45), head and neck (HR = 1.08; 95% CI, 1.01-1.17), and acute myeloid leumkemia (HR = 1.14; 95% CI,1.00-1.30).
Long sleep had associations with elevated risk for several cancers, though none were statistically significant.
Individuals who reported restless sleep had a significantly higher risk for hepatocellular carcinoma (HR = 1.31; 95% CI, 1.03-1.67), but a significantly lower risk for breast cancer (HR = 0.95; 95% CI, 0.9-0.99). Restless sleep also had an association with lower rectal cancer risk (HR = 0.78; 95% CI, 0.63-0.96), but those data only included two cohorts.
Researchers did not observe any association between trouble sleeping and cancer risk.
Zhong acknowledged study limitations, including patients self-reporting their sleep habits.
Researchers plan to add eight additional cohorts into their meta-analysis to develop a “clearer picture” of these findings, Zhong added.
“At the moment, only about 5% of participants reported long sleep,” Zhong said. There has always been this assumption that short sleep is bad, but more studies are showing that longer sleep may be worse.”
Future investigations are needed to understand why short sleep duration and/or disrupted sleep may lower risk for some cancer.
“Timing of sleep also is really important,” Zhong said. “It’s not just how much you sleep, it’s if you’re also going to sleep at an appropriate time, with consistency, and if that aligns to your body’s appropriate time.”
These studies can be difficult to conduct, but technology could revolutionize the research.
“There are a lot of wearables and nearables,” Zhong said. “Everything from watches, rings, even beds that tracks your sleep. All these data are being collected, and if we could tap into it, and get those more objective measures, that would be amazing.”
For more information:
Charlie Zhong, PhD, MPH, can be reached at charlie.zhong@cancer.org.
<












Leave a Reply