January 23, 2026
3 min read
Key takeaways:
- Combining two health care systems, the odds for penicillin allergy delabeling were significantly reduced among Black vs. white patients.
- After being separated, the opposite was found in one health system.
The likelihood for penicillin allergy delabeling was significantly reduced among Black and Asian patients vs. white patients, but this changed based on health system, according to data published in Annals of Allergy, Asthma & Immunology.

Data were derived from Blumenthal KG, et al. Ann Allergy Asthma Immunol. 2025;doi:10.1016/j.anai.2025.11.025.

Kimberly G. Blumenthal

Alysse G. Wurcel
“We appreciate the limitations of race and ethnicity as classifications, especially in electronic health records; however, we were surprised that race and ethnicity had variable associations depending on the hospital system,” Kimberly G. Blumenthal, MD, MSc, professor of medicine at Mayo Clinic College of Medicine and Science, and Alysse G. Wurcel, MD, MS, associate professor of medicine at Boston University School of Medicine, told Healio in a statement.
“Within one hospital system, Black patients were more likely to be delabeled, but within another hospital system, Black patients were less likely to be delabeled,” they said.
Using electronic health record data from January 2019 to April 2022, Blumenthal and colleagues evaluated 77,047 primary care patients with any active or inactive penicillin allergy record at two health care systems (Mass General Brigham and Tufts Medicine) to uncover if there is a difference in penicillin allergy delabeling prevalence based on race.
“It is known that penicillin allergy evaluation and delabeling improves clinical care, but access to delabeling is often limited to specialist allergy visits, which may not be routinely accessible,” Blumenthal and Wurcel said. “There is also robust literature about how people’s race and ethnicity can impact access to health care.
“The association with race and ethnicity with access to penicillin allergy delabeling needed more investigation,” they continued.
A small proportion of patients in the total population were delabeled (6.8%), according to the study.
In the Mass General Brigham group (n = 46,854; median age, 58 years; 70% women; 80% white; 6% Black; 4% Asian), 10% of patients were delabeled, which was significantly greater than the 3% of patients in the Tufts Medicine group (n = 30,193; median age, 58 years; 69% women; 82% white; 4% Black; 5% Asian).
Researchers noted that allergy/immunology visits were where most patients at Mass General Brigham underwent penicillin allergy delabeling (47%), and this differed from Tufts Medicine where primary care visits were where most patients underwent delabeling (43%). Delabeling during allergy/immunology visits was reported for 5% of patients at Tufts Medicine, and delabeling during primary care visits was reported for 20% of patients at Mass General Brigham.
Considering both systems, the odds for penicillin allergy delabeling were significantly reduced among Black vs. white patients (adjusted OR = 0.73; 95% CI, 0.64-0.84) and Asian vs. white patients (aOR = 0.76; 95% CI, 0.65-0.88).
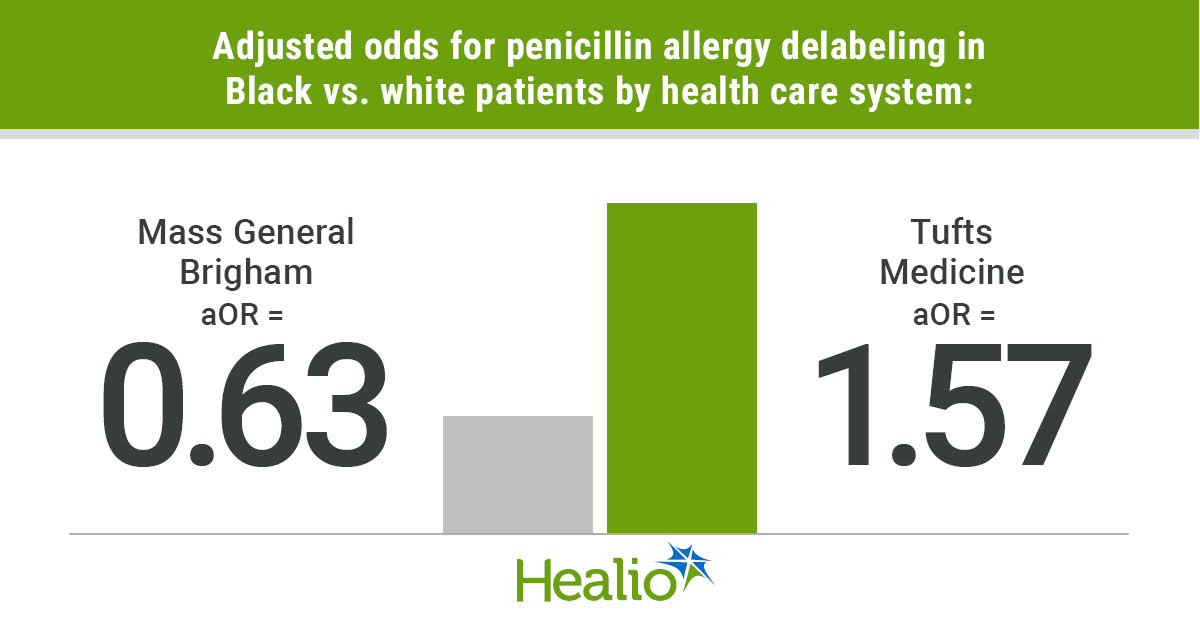
When broken down by health system, researchers continued to find significantly decreased odds for delabeling among Black vs. white patients (aOR = 0.63; 95% CI, 0.54-0.73) and Asian vs. white patients (aOR = 0.74; 95% CI, 0.63-0.88) in the Mass General Brigham group.
Among Tufts Medicine patients, the link between Asian race and reduced odds for delabeling did not reach significance. Additionally, the odds for delabeling were significantly increased among Black vs. white patients in this health system (aOR = 1.57; 95% CI, 1.18-2.1), according to the study.
“We found differences in delabeling for Black patients between institutions,” Blumenthal and Wurcel told Healio.
“We are intrigued by the heterogeneity,” they added. “The next step of our research aims at digging in deeper to differences between institutions, such as availability of allergists, comfort of primary care clinicians with delabeling in ambulatory practices and other potentially important factors.”
Researchers did not observe any significant mediators in the link between Black race and lower odds for penicillin allergy delabeling among patients from Mass General Brigham. In contrast, the relationship between Asian race and delabeling prevalence was “partially explained” by two mediators: non-English language preference (8%) and health care visits (up to 16%).
Switching to patients from Tufts Medicine, the study identified two mediators in the link between Black race and elevated odds for delabeling: Health care visits (15%; allergy/immunology visits, 39%; inpatient visits, 8%; emergency visits, 7%) and Charlson Comorbidity Index (CCI; 10%).
Similar to Mass General Brigham, researchers found that the relationship between Asian race and delabeling prevalence was mediated by non-English language preference (61%) and health care visits (37%; inpatient visits, 9%; emergency visits, 13%), as well as CCI (7%).
“We found that an important barrier to penicillin allergy delabeling is non-English language preference for Asian patients,” Blumenthal and Wurcel told Healio. “This means that one of the reasons that Asian people may not be getting delabeling is because of the language barrier between patients and doctors.
“Future studies should seek to understand the barriers and facilitators to delabeling and uncover methods to improve access to, and uptake of, penicillin allergy delabeling,” Blumenthal and Wurcel added.
For more information:
Kimberly G. Blumenthal, MD, MSc, can be reached at blumenthal.kimberly@mayo.edu.
Alysse G. Wurcel, MD, MS, can be reached at alysse.wurcel@bmc.org.
<













Leave a Reply