April 14, 2026
1 min watch
Key takeaways:
- Lower-than-recommended levels of moderate to vigorous physical activity can significantly improve cancer survival.
- Exercise improved rectal and lung cancer survival among those who were inactive before diagnosis.
Engaging in moderate to vigorous physical activity, even below recommended levels, can significantly improve cancer survival for multiple malignancies.
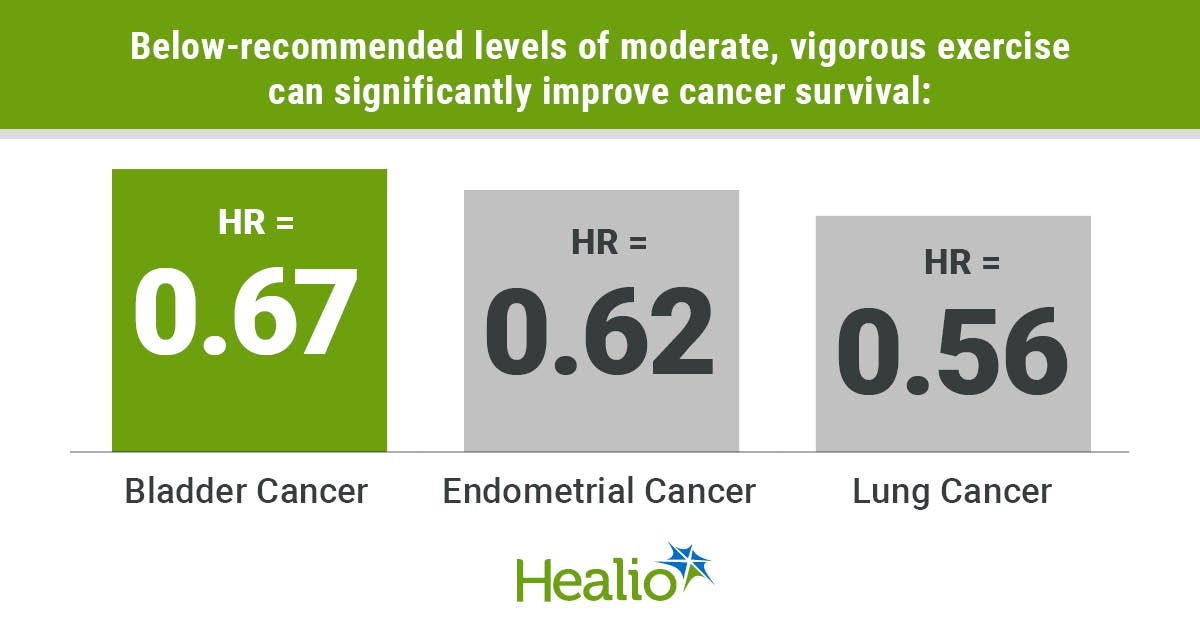
An evaluation of more than 17,000 patients showed less than 75 minutes of moderate to vigorous exercise per week could reduce the risk for death for bladder, endometrial and lung cancers, and reaching recommended exercise levels could enhance those benefits.

Data derived from Rees-Punia E, et al. JAMA Netw Open. 2026;doi:10.1001/jamanetworkopen.2025.56971.
Additionally, individuals with lung cancer or rectal cancer who did not exercise prior to their diagnosis could significantly improve their survival with recommended moderate to vigorous physical activity after their diagnosis.

Alpa V. Patel
“Encourage your patients that doing something is better than doing nothing, and doing more is better,” Alpa V. Patel, PhD, senior vice president of population science at American Cancer Society, told Healio.
‘Scientific evidence’
Healio previously reported on multiple studies that showed the benefits of exercise on cancer outcomes, including how 7,000 steps per day significantly decreased cancer mortality, and that exercise after surgery and adjuvant chemotherapy significantly decreased the risk for recurrence or death among patients with colon cancer.
Individuals who have a history of cancer are advised to do 150 to 300 minutes of moderate intensity or 75 to 150 minutes of vigorous intensity aerobic activity every week, according to study background.
However, these recommendations were developed based on studies evaluating breast, colorectal or prostate cancer.
“I would love for physical activity to be important for every single type of cancer, but depending on what the causes of that particular cancer are, whether physical activity is beneficial is really going to be driven by the underlying biology,” Patel said. “It’s important for us to be able to understand that.
“It’s also really important to be able to say there is scientific evidence of the benefits of exercise for your cancer. That is likely to motivate engagement in exercise more than just the general, it’s good for your health, it’s good for cancer survival.”
Patel and colleagues previously found engagement in recommended levels of moderate to vigorous physical activity significantly improved survival compared with no exercise for a variety of malignancies, including oral, endometrial, lung, rectal, respiratory, bladder, kidney, prostate, colon and breast cancers.
They conducted another investigation evaluating lesser-studied malignancies and the dose response of exercise.
The pooled analysis from six different cohorts included 17,141 survivors (mean age, 67 years; standard deviation, 8; 60% women) with bladder, endometrial, kidney, lung, oral cavity, ovarian or rectal cancer.
The most common malignancies included bladder (24%), endometrial (22%) and lung cancers (18%).
The association of moderate to vigorous physical activity on survival served as the primary endpoint.
‘The one you’ll keep doing’
After mean follow-up of 10.9 years, 4,872 individuals died of cancer.
Compared with those who reported no physical activity, patients who engaged in any physical activity following their diagnosis had significantly lower risk for death from bladder (HR = 0.67; 95% CI, 0.5-.91), endometrial (HR = 0.62; 95% CI, 0.45-0.87) and lung cancers (HR = 0.56; 95% CI, 0.43-0.75).
Meeting guideline recommendations for moderate to vigorous physical activity further reduced mortality risk for endometrial (HR = 0.4; 95% CI, 0.21-0.78) and lung cancer (HR = 0.38; 95% CI, 0.24-0.6) compared with no activity.
Doubling those recommendations significantly improved survival for oral (HR = 0.39; 95% CI, 0.15-0.99) and rectal cancer (HR = 0.57; 95% CI, 0.33-0.97).
Among patients who did not engage in physical activity before diagnosis, meeting guidelines after cancer significantly reduced mortality from lung (HR = 0.58; 95% CI, 0.47-0.71) and rectal cancer (HR = 0.51; 95% CI, 0.32-0.83).
“So often you do hear cancer survivors say, ‘I haven’t engaged yet. I haven’t had a really active lifestyle,’” Patel said. “These types of data are really exciting to me because it reinforces that it’s never too late to get started. If people ask, ‘What kind of exercise should I be doing?’ My answer is always, ‘The one you’ll keep doing,’ because doing exercise throughout your life course is the most beneficial.
“I’m often asked by clinicians, ‘What should I be telling my patients?’” she added. “I say, ‘Put a pair of sneakers on and walk 30 minutes a day, 20 minutes a mile.’ That’s all I’m asking for. I’m not asking you to go become a marathon runner. I’m asking for you to build up to 30 minutes of a 3-mile-an-hour pace, five times a week. That has tremendous health benefits for cancer, for cardiovascular disease, for diabetes, for stroke, and so much more.”
Researchers acknowledged study limitations, including the potential for inactivity to be an indication for poor general health or being closer to death, which could affect the associations between physical activity and survival.
‘It’s critical’
As more studies show the benefits of exercise on cancer outcomes, future research should continue to refine dose and timing of physical activity on various malignancies.
“How can we get to the precision of dosing physical activity?” Patel asked.
Patel referenced a study Healio previously reported on, which showed walking could help mitigate increased mortality risk certain women with breast cancer may have based on higher genetic predisposition to obesity.
“We often hear, ‘I just have bad genes,’” Patel said. “Here is this actionable message that we can deliver to a survivor and say, ‘You can overcome those ‘bad genes’ by doing exercise. You just may need to walk a little bit more.’”
Technology could help provide data to personalize exercise approaches.
“So many people are monitoring physical activity with devices,” Patel said. “Can we actually look at what 24-hour movement behavior looks like? Is there a time of day where you optimize the benefits of physical activity? How does it need to be distributed? Being able to more finely measure physical activity through device-based measurements is going to help us do that type of work at scale in a way that we’ve never been able to before.”
Those data could help achieve the ultimate goal, having insurance cover exercise programs.
“It’s critical. We have to put the measures in place that support individuals to be able to practice these nontherapeutic or nonpharmacologic interventions,” Patel said. “Coverage is going to be essential to that. That’s exactly what we need to be focusing on. How do we actually provide guidance around coverage for exercise therapy in cancer care and longer term? For most people, that is a huge challenge.
“If we would have tried to get to behavior change an individual at a time with cigarette smoking, we wouldn’t have seen the tremendous impact we’ve had in tobacco control over the last few decades,” she added. “That has happened because there was taxation around cigarettes. There are smoke-free laws that prevent all the places in public where you can smoke. There is coverage in many types of insurance policies around smoking cessation products. Those types of things allow and enable, at scale, for that type of behavior change, and it is going to be an essential component in this.”
For more information:
Alpa V. Patel, PhD, can be reached at alpa.patel@cancer.org.
<












Leave a Reply