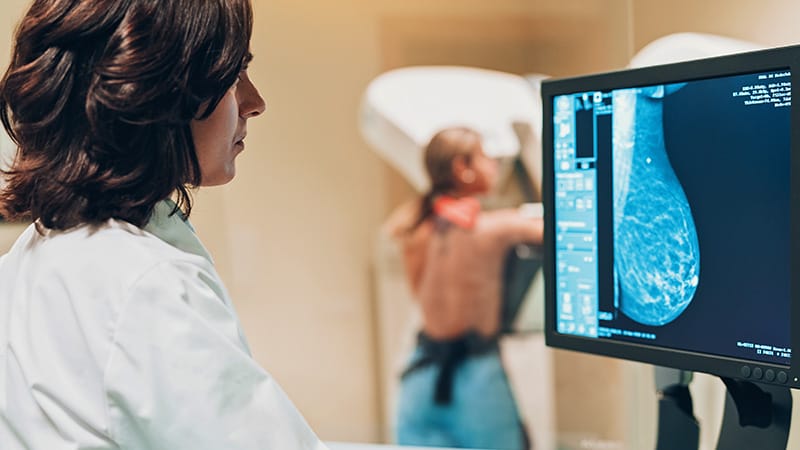
The American College of Physicians (ACP) has updated its guidance on screening for breast cancer in asymptomatic average-risk women using recent high-quality clinical recommendations from guideline developers from expert societies around the world.
Publishing in the Annals of Internal Medicine, panelists led by Amir Qaseem, MD, PhD, MHA, the ACP’s chief scientific officer and senior vice president of clinical policy, made five recommendations, taking into account age group and breast density category.

“This updated guidance statement is based on new data and new or updated guidelines evaluated by the ACP since the publication of our 2019 guidance statement, which is over 7 years old,” Qaseem told Medscape Medical News.
“Our guidance is for asymptomatic, average-risk females,” he stressed. “It does not apply to adult females who have breast cancer symptoms or are at higher risk for breast cancer.” These include those with a personal history of breast cancer or diagnosis of a high-risk breast lesion, a known genetic abnormality such as BRCA1 or BRCA2, another familial breast cancer risk syndrome, or a history of high-dose radiation therapy to the chest at a young age.
First, the 2026 guidance recommends that clinicians screen women aged 50-74 years with biennial mammography. About 80% of US women aged 50-74 years currently undergo biennial mammography. Adults who undergo annual mammography have a 50%-60% chance of a false positive result over 10 years.
Second, for women aged 40-49 years, the guidance recommends a shared decision-making approach with discussion of the individual woman’s risk for breast cancer, her values and preferences, and uncertainty around the benefits and harms of breast cancer screening.
“It’s a personal choice,” said Qaseem. “The key discussion points include the small absolute reduction in mortality but no difference in advanced breast cancers. This needs to be balanced against harms.”
Harms include overdiagnosis, overtreatment, false negatives, increased risk for additional tests and radiation exposure, false positive-related psychological distress, and false positive results that reduce adherence to future screening.
Third, for those aged 75 years or older — or with a limited life expectancy — the new advice recommends the use of shared decision-making regarding screening discontinuation and uncertainty around benefits and harms.
Fourth, clinicians should consider using supplemental digital breast tomosynthesis in women with a potentially lesion-obscuring breast density category on the Breast Imaging Reporting and Data System (BI-RADS).
This category includes C (heterogeneous mix of fatty but mainly dense fibroglandular tissue) or D (mainly dense tissue).
And fifth, the new guidance notably recommends against using supplemental MRI or ultrasound in women with a breast density BI-RADS category C or D.
The ACP guidance statement supports earlier recommendations against breast self-examination owing to the risk for false positives.

“These are very thoughtful and reasonable recommendations based on new data,” said Boston internist Mara A. Schonberg, MD, MPH, a professor of medicine at Harvard Medical School and director of research in shared decision-making in the Division of General Medicine at Beth Israel Deaconess Medical Center, in comments to Medscape Medical News. They address a number of issues based on data from mixed study types from randomized controlled trials and observational studies to modeling data, she added.
They also assume that women are capable of making their own decisions about mammography. “Unfortunately, some societies have the paternalistic attitude that all women should be screened every year from age 40 on.”
While many women are still being screened early, no trial data show an overall mortality benefit, Schonberg said. “Early mammography may find a slow-growing cancer, but after 30 years, a woman is more likely to die of other causes like cardiovascular disease.”
Financial support came exclusively from the ACP’s operating budget. The authors had no relevant conflicts of interest to disclose. Schonberg reported reviewing for UpToDate.
<











Leave a Reply