April 23, 2026
5 min read
Key takeaways:
- Younger nonsmokers with lung cancer followed a healthier diet than the general population.
- Exposure to pesticide residue on fruits, vegetables and whole grains may be driving lung cancer risk in this group.
A study designed to investigate why lung cancer incidence has increased among younger nonsmokers over the past few decades yielded a surprising observation.
Data from nearly 200 people diagnosed with lung cancer prior to age 40 revealed they adhered to a healthier diet than the general U.S. population.

Data derived from Gorbatov SD, et al. Abstract 5039. Presented at: American Association for Cancer Research Annual Meeting; April 17-22, 2026; San Diego.

Jorge Nieva
The finding suggests an environmental risk factor — possibly residue from pesticides used to protect commercially produced crops from disease, weeds or pests — could be contributing to the trend, Jorge Nieva, MD, medical oncologist and lung cancer specialist at USC Norris Comprehensive Cancer Center, and colleagues concluded.
“A healthy diet is very important, but people who consume diets that are high in fruits, vegetables and whole grains consume about three times the average pesticide exposure as people who eat a standard American diet,” Nieva told Healio. “It makes us wonder if something in food is driving this.”
‘What is going on?’
In the 1980s, multiple reports by U.S. Surgeon General C. Everett Koop, MD, FACS, emphasized the detrimental health impacts of smoking and exposure to second-hand smoke.
The percentage of U.S. adults who smoked cigarettes, already on the decline from a peak of about 45% in the 1960s, dropped sharply until reaching an all-time low of 9.9% in 2024.
As smoking declined, so did lung cancer incidence nationwide — except among nonsmokers aged 50 years or younger.
Cancers among younger individuals are biologically distinct from lung cancer in older adults. They often harbor actionable driver mutations, such as EGFR mutations or ALK rearrangements, and they disproportionately affect women.
“Men and women stopped smoking at approximately the same rate, but incidence of lung cancer among men declined while incidence among women did not. Women have not had what I call the smoking cessation dividend,” Nieva said. “We’re now seeing around 20,000 to 25,000 lung cancer deaths in the United States each year among nonsmokers. That is more than non-Hodgkin lymphoma or leukemia, so it certainly is not rare. We need to start asking what is going on and what has changed.”
Nieva and colleagues hypothesized that an alternative carcinogenic pathway — one that likely emerged around the mid-1980s and has greater effect on women — could be involved.
Researchers collaborated with the Addario Lung Cancer Medical Institute and GO2 for Lung Cancer to launch the multi-institutional, observational Epidemiology of Young Lung Cancer study.
At this year’s American Association for Cancer Research Annual Meeting, Nieva and colleagues presented findings from an analysis of 187 people (78.1% women; 76.4% non-Hispanic white) diagnosed with non-small cell lung cancer prior to age 40.
Participants completed epidemiological surveys that assessed demographics, physical activity, smoking history and oral contraceptive use. They also completed validated food frequency questionnaires.
Researchers obtained information about tumor genomics and classified study participants by biological pathway of driver mutations, with 43.9% classified as fusion positive (ALK, ROS1, RET or NTRK), 39% classified as having mutations in the EGFR pathway, and 17.1% determined to have other or mixed mutations (eg, KRAS, BRAF, MET, etc.).
Making the connection
About 70% of participants overall had never smoked, though percentages varied by pathway group (EGFR, 60.3%; fusion positive, 79.3%; other/mixed, 68.8%).
“The epidemiologic surveys did not show anything that stood out as an obvious or conventional exposure, such as radon or something related to the part of the country where they grew up,” Nieva said.
However, when researchers assessed diet quality using the Healthy Eating Index (HEI)-2020 — a measure of how well food consumption aligns with recommendations in national dietary guidelines — they observed an unusual pattern.
Results showed higher HEI-2020 scores — based on a 100-point scale — among those in the EGFR pathway group (64.94) and fusion-positive group (65.26) than the national average (57) as calculated from National Health and Nutrition Examination Survey questionnaires. Women had higher scores than men.
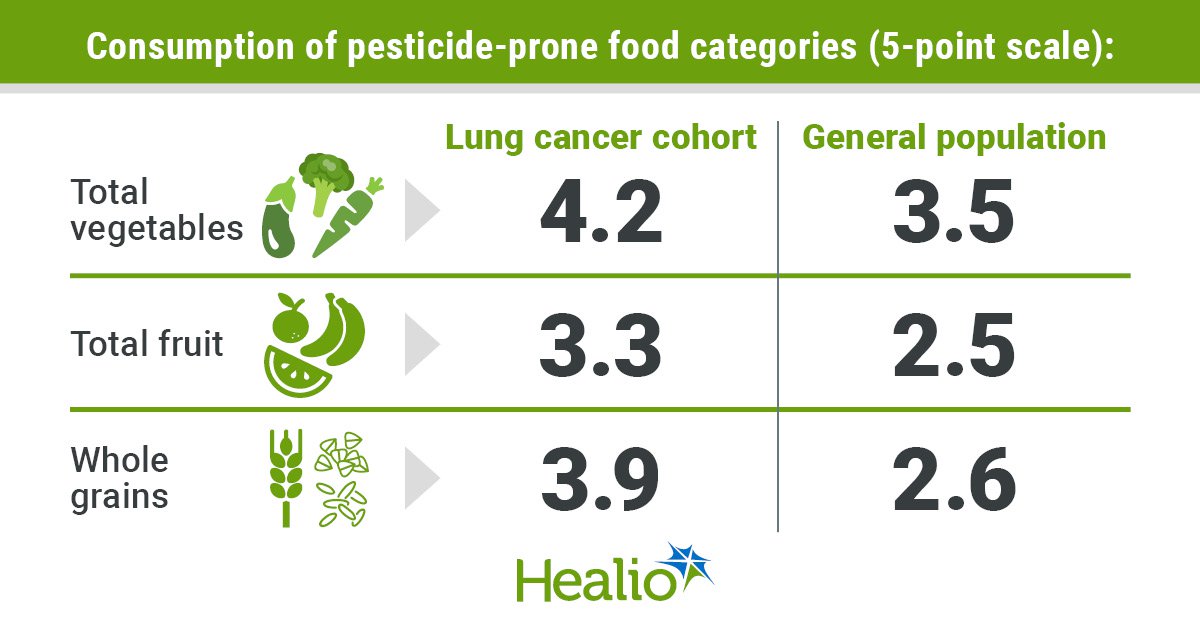
In addition, a comparison of HEI component scores— measured on 5-point scales — revealed higher consumption of pesticide-prone food categories in the study cohort than the general population. This finding remained consistent for consumption of total vegetables (4.2 vs. 3.5), dark green vegetables and legumes (4.3 vs. 3.6), total fruit (3.3 vs. 2.5), whole fruit (3.9 vs. 3.8) and whole grains (3.9 vs. 2.6).
“This was not an association we were really looking for, and it’s not something we expected,” Nieva said. “It is counterintuitive.”
The hypothesis that elevated pesticide exposure may contribute to lung cancer risk among individuals who consume more fruit, vegetables and whole grains is strengthened by prior research that examined the impact of certain occupational exposures.
Findings from a study published in Occupational & Environmental Medicine showed agricultural workers who use pesticides have more than double the risk for lung cancer than the general population (HR = 2.38; 95% CI, 1.07-5.28).
“I don’t think we would have made the connection [between diet and lung cancer] if it weren’t for the prior study of occupational exposure among pesticide sprayers,” Nieva said.
‘An epidemic’
Nieva and colleagues reported “consistently elevated” use of oral contraceptives among the young individuals with lung cancer.
Oral contraceptives contain progestin and estrogen. These synthetic hormones act as endocrine disruptors to prevent ovulation.
Many pesticides also fall into the category of endocrine-disrupting chemicals, which interfere with the body’s hormonal system and also can interact with estrogen receptors frequently observed in lung cancers among younger individuals.
“Our hypothesis is that one of the endocrine-disruptive chemicals is leading to signaling growth and proliferation, and that may be what is causing lung cancer in young people,” Nieva said.
For now, washing fruits and vegetables — and purchasing organically grown food — can help reduce the potential risks of pesticide exposure, Nieva said.
More investigation will be necessary to clarify if or how these chemicals affect lung cancer risk among younger individuals. A key next step will be getting “more drilled-down exposure histories” and using blood or urine samples to measure levels of specific chemical entities, Nieva said.
This type of work ultimately could inform lung cancer prevention strategies or public health recommendations, but funding will be essential to move research forward, Nieva said.
“We have a Health and Human Services secretary who is very interested in healthy habits and the connection between lifestyle and disease,” Nieva said. “My hope is that this spawns a desire to provide grants or other funding for very exciting research projects around this hypothesis and explore what amounts to an epidemic that shouldn’t be there.
“It’s hidden, because lung cancer incidence is going down,” he added. “Everybody thinks we’re doing a great job with lung cancer because we’re seeing fewer cases and people aren’t smoking as much. But we’re not recognizing that cases among nonsmokers are going up, and we need to understand why.”
For more information:
Jorge Nieva, MD, can be reached at jorge.nieva@med.usc.edu.
<











Leave a Reply