April 29, 2026
3 min read
Key takeaways:
- Nearly 15% of acute coronary syndrome cases at a Northern California safety-net hospital system are meth-related.
- Meth-related ACS was more prevalent among younger men with poor social determinants of health.
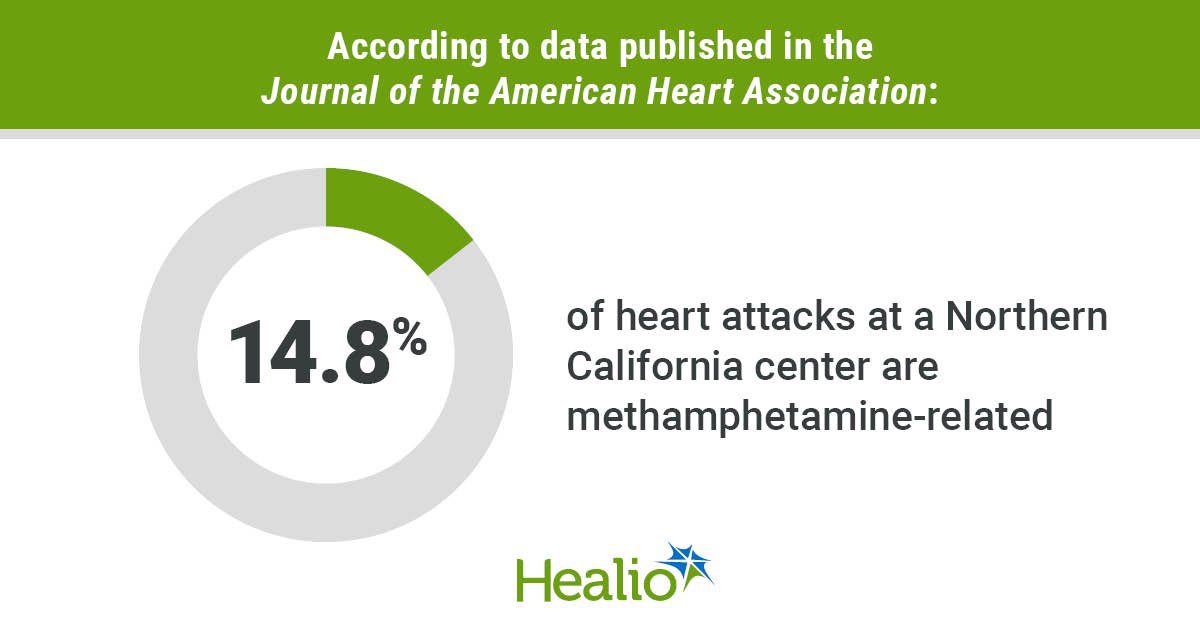
Nearly 15% of acute coronary syndromes in Northern California are methamphetamine-related, which remains a strong predictor of poor survival in a population of predominantly young men, researchers reported.
Despite lower levels of traditional risk factors such as diabetes and obesity, patients with methamphetamine-associated ACS experience significantly higher rates of all-cause mortality compared with nonusers with ACS, according to data published in the Journal of the American Heart Association.

Data derived from Zhao SX, et al. J Am Heart Assoc. 2026;doi:10.1161/JAHA.125.046514.
“The key takeaway for my cardiology colleagues is the need for heightened awareness of the strong association between methamphetamine and ACS, the particularly severe outcomes observed in this population and the importance of tailored counseling and treatment strategies,” Susan Zhao, MD, associate division chief of cardiology and medical director of the coronary care unit at Santa Clara Valley Medical Center in San Jose, California, and an associate clinical professor of medicine (affiliated) at Stanford University School of Medicine, told Healio. “Methamphetamine cessation should be emphasized as a critical component of secondary prevention, in addition to the standard measures of adopting a heart-healthy lifestyle and adhering to guideline-directed cardiac medications. Incorporating methamphetamine use screening, cessation support and close follow-up represents a unique and essential dimension in the care of this high-risk population.”
Researchers estimated the prevalence of methamphetamine-associated ACS using patient data from the public safety-net Santa Clara Valley HealthCare system gathered between 2012 and 2022.
Eligible patients were adults younger than 65 years who presented with ACS attributed to type I MI. Methamphetamine use was determined by patient self-report or detection on urine toxicology screen, and concomitant cocaine users were excluded, according to the study methods.
“My team has been studying methamphetamine-associated cardiac diseases for over 10 years at our hospital, which serves as the safety-net hospital for the county of Santa Clara in Northern California, where methamphetamine use is highly prevalent,” Zhao told Healio. “We published multiple reports on the two most common and well-described conditions linked to long-term methamphetamine use, namely HF and pulmonary arterial hypertension. Acute heart attack in the setting of methamphetamine use is less well known, but we believe it occurs more often than is currently reported. That’s why we undertook this project to systematically characterize this group of patients who suffered heart attack in the setting of meth use. “
ACS cases in Northern California
Among 1,309 patients who presented with ACS, 14.8% of cases were methamphetamine-related, according to the study.
Researchers reported that patients with methamphetamine-associated ACS were less frequently women (14.9% vs. 24.8%; P = .022) and with younger median age (52 years vs. 57 years; P < .001) compared with nonusers.
Patients with methamphetamine-associated ACS more often presented with nonobstructive coronary diseases vs. nonusers (24.2% vs. 10.6%; P < .001), according to the study.
During a median follow-up of nearly 52 months, in an unadjusted analysis, all-cause mortality was higher among patients with methamphetamine-associated ACS vs. nonusers (HR = 1.61; 95% CI, 1.15-2.25; P = .006) and, after adjustment for confounding variables, methamphetamine use was the strongest independent predictor of all-cause mortality in patients with ACS (HR = 2.08; 95% CI, 1.4-3.09; P < .001), according to the researchers.
Risk factors in meth-related ACS
Researchers observed that, despite being at younger median age, patients with methamphetamine-associated ACS had similar rates of hypertension, obesity, prior atrial fibrillation and prior stroke compared with nonusers with ACS.
Patients with methamphetamine-associated ACS had lower rates of diabetes (37.6% vs. 51%; P = .001) and more favorable creatinine (1.16 mg/dL vs. 1.5 mg/dL; P = .018), total cholesterol and LDL levels (P for both = .005), according to the study.
The rates of homelessness (25.8% vs. 3.2%; P < .001), current alcohol use (28.9% vs. 8.3%; P < .001) and current cigarette smoking (71.6% vs. 27.6%; P < .001) were all higher in the methamphetamine-associated ACS group vs. the nonuser group, according to the study.
“We hypothesized that meth-related ACS would differ from non-meth ACS. This was confirmed by the results of the study, which came as no surprise,” Zhao told Healio. “Building on our prior work in HF and pulmonary hypertension, we have consistently observed that, at similar level of disease severity, patients with methamphetamine use experience worse outcomes than those without. Our current findings align with these previous observations across the spectrum of methamphetamine-related CVD.
“Given the retrospective, single-center design of this study, we cannot draw causal inferences,” Zhao told Healio. “Meth use may serve as a marker for poorer outcomes due to associated social determinants of health, in addition to its direct mechanistic effects on the CV system.”
For more information:
Susan Zhao, MD, can be reached at cardiology@healio.com.
<










Leave a Reply