April 18, 2026
3 min read
Key takeaways:
- Musculoskeletal issues can typically be diagnosed on clinical exam.
- Physical therapy is the mainstay treatment. Corticosteroids can be used to supplement — not replace — physical therapy.
SAN FRANCISCO — Most musculoskeletal issues can be managed in primary care as they typically do not require complex imaging or immediate specialist referral, according to a speaker here.
Common musculoskeletal conditions include lateral hip pain, anterior knee pain, ankle inversion injuries, shoulder pain, stiff shoulders and lateral elbow pain, Joshua T. Goldman, MD, MBA, associate clinical professor in the division of sports medicine at the University of California, Los Angeles, told attendees at ACP’s Internal Medicine Meeting.

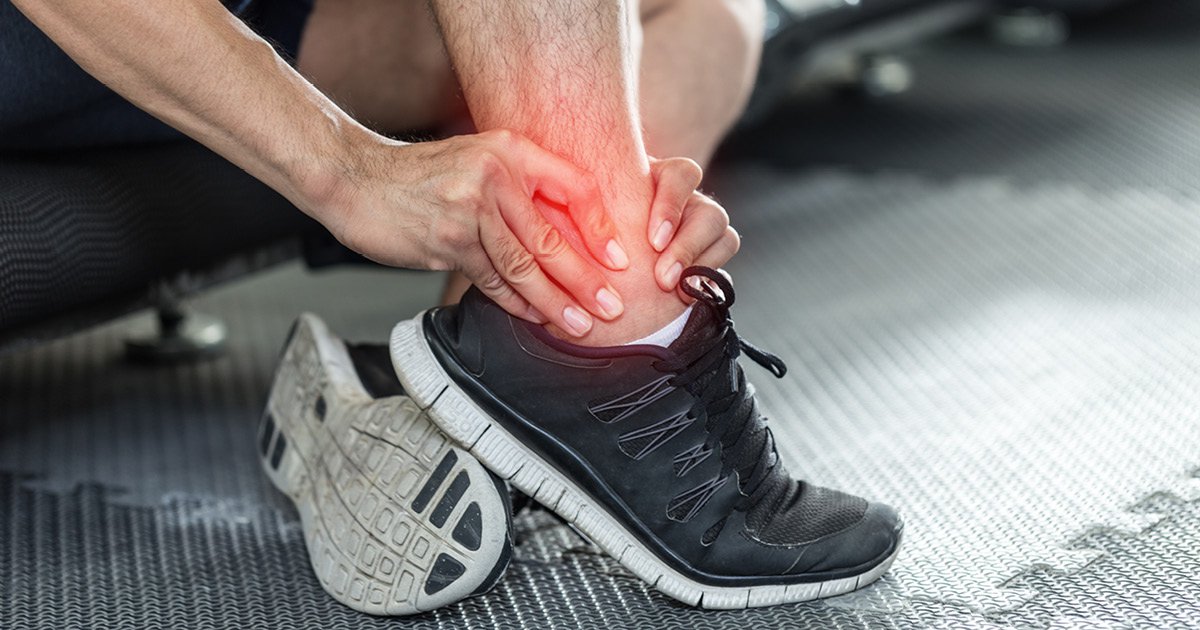
Ankle sprains accounted for about 7% to 10% of ED visits, according to Joshua T. Goldman, MD, MBA. Image: Adobe Stock
Understanding how to diagnose and manage these conditions can potentially reduce ED overuse. For example, “one ankle inversion injury is occurring per 10,000 people each day. Ankle sprains constitute 7% to 10% of all visits to the ED. So, if we’re trying to declutter our ERs, this is a good place to start,” Goldman said.
He outlined some practical tips for primary care physicians to keep in mind when approaching musculoskeletal injuries:
- Most diagnoses can be made with a clinical exam. Goldman advised primary care providers to “trust your targeted history and exam.” Although imaging is a helpful adjunct, advanced imaging may show abnormalities not related to the patient’s symptoms. For example, he said “there’s nothing more terrifying than MRI’ing the foot of a middle-aged runner. You’re going to see a lot of bad stuff in there. I warn patients … it’s going to look bad. Don’t freak out.”
- “-itis” is often a misnomer. Many conditions are not primarily inflammatory but instead are often caused by tissue degeneration, Goldman said. For example, “greater trochanteric pain syndrome is actually gluteal tendinosis, and lateral epicondylitis is actually common extensor tendinosis,” he said. “When we start to reframe what that pathology is, the treatment starts to make more sense.”
- Biomechanics drive symptoms. Underlying mechanical issues like muscle weakness are often the root cause of pain. Passive interventions alone cannot resolve the issue; the biomechanics need to be corrected, Goldman said.
- “Physical therapy is the cornerstone of treatment.” Most patients with musculoskeletal issues benefit from physical therapy, according to Goldman. But PCPs must “be specific, be prescriptive and be targeted” in what they want the physical therapist to work on, not just “‘PT, shoulder pain,’” he said. Tendons in particular need “eccentric and progressive loading,” Goldman said. “We’re taught if it hurts, don’t do it. We say that a lot to patients about their pathologies. Tendons are the exception. You need to grit it out, because if you don’t load the tendon, it’s not going to repair …. Soreness is actually part of that healing process.”
- Corticosteroids are “useful but limited.” Although they provide pain relief, corticosteroid injections often have inferior long-term outcomes, “especially for tendon pathology,” Goldman said. “For a long, long time, we believed they were curative, [which is] not true,” he added. Goldman recommended using corticosteroid injections as an adjunct to physical therapy, not as a replacement, “with the exception of frozen shoulder, specifically.”
- Early mobilization is better than immobilization. The traditional “rest, ice, compression and elevation” approach can be used “for a little bit,” but Goldman said “you have got to get moving.” For ankle sprains specifically, “we need to strengthen [and] fix the biomechanics,” he said. “Give them a little supportive care with an ankle brace for that first week, but then you have got to get them out and get them into rehab.”
- “Know when to escalate care.” Goldman advised referring patients to a specialist when they are not improving with structured rehabilitation or if there is concern about structural pathology like a tendon tear. “Get your advanced imaging. Feel free to refer them on for additional care,” he said. “I always tell my fellows, if you look at an X-ray and you freak out, just send it to somebody else. That’s totally fine.”
<









Leave a Reply