April 17, 2026
4 min read
Key takeaways:
- OCT and cardiac MRI often enabled diagnosis of a MI cause in patients without blocked arteries.
- Coronary function testing usually identified a vasomotor disorder in those with ischemia but no blocked arteries.
NEW ORLEANS — Two studies presented at the American College of Cardiology Scientific Session offered insights into how to diagnose and treat patients with heart disease but not blocked arteries.
In the HARP trial, researchers found that using optical coherence tomography (OCT) plus cardiac MRI led to a causal diagnosis in 79% patients with MI with nonobstructive coronary arteries (MINOCA).

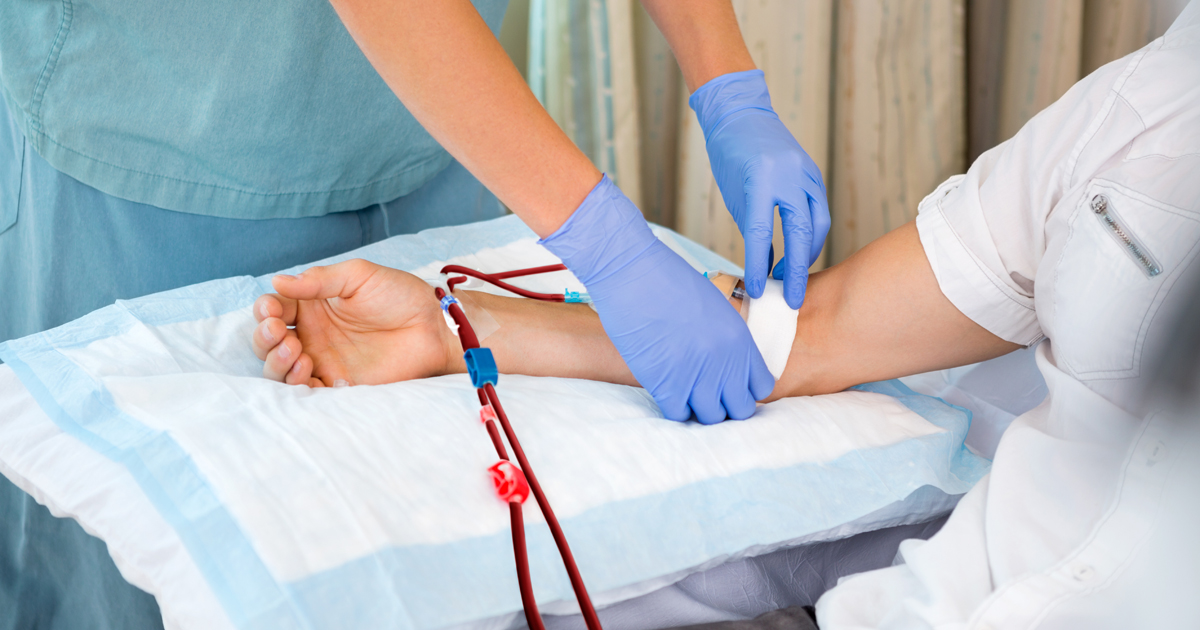
OCT and cardiac MRI often enabled diagnosis of a MI cause in patients without blocked arteries. Image: Adobe Stock
In the DISCOVER-INOCA trial, standardized invasive coronary function testing determined that 94% of patients with ischemia with nonobstructive coronary arteries (INOCA) had a coronary vasomotor disorder and enabled reclassification of the initial diagnosis for 89% of patients.
HARP

Harmony R. Reynolds
For HARP, Harmony R. Reynolds, MD, Joel E. and Joan L. Smilow Professor of Cardiology at NYU Grossman School of Medicine and director of the Center for Women’s Cardiovascular Health and associate director of the Cardiovascular Clinical Research Center at NYU Langone Health, and colleagues enrolled 754 patients who had a clinical diagnosis of MI and were referred to the cath lab but had no known coronary artery disease.
“We were hoping that we would be able to not only identify underlying causes of MINOCA, but that we would be able to use clinical or MI characteristic predictors in order to figure out who benefits the most from imaging, where the diagnostic yield is highest,” Reynolds told Healio. “And we also had hoped that we would be able to define sex differences, because after all, MINOCA is so much more common among women than men when they have MI.”
The initial cohort included 539 women and 215 men. OCT screening was performed in 270 women and 66 men (median age, 58 years; median peak troponin level, 32 times the upper reference limit of normal), and cardiac MRI was performed and interpretable in 225 women and 59 men. The top reasons for screen failure were diagnosis of CAD with stenosis 50% or more in 36% of women and 61% of men, no OCT performed in 8% of women and 2% of men and diagnosis of spontaneous coronary artery dissection on angiography in 4% of women and 2% of men.
OCT identified a culprit lesion in 45% of patients, plaque rupture in 7% of patients, intraplaque hemorrhage in 17%, healed plaque in 12%, plaque erosion in 5%, a calcified nodule in 2%, thrombus without plaque in 1% and spontaneous coronary artery dissection in 0.6%, Reynolds and colleagues found.
The percentage of patients with a culprit lesion identified by OCT did not differ by sex (women, 44%; men, 53%; P = .18), a culprit lesion was less likely to be identified in patients who had normal coronary angiography than in those with any angiographic stenosis (27% vs. 61%; P = .003) and predictors of a culprit lesion included older age, angiographic stenosis and 3-vessel OCT imaging, Reynolds said during a presentation.
Among patients who had cardiac MRI (median time after OCT, 6 days), 37% had normal findings, 28% had an infarction, 12% had a regional injury and 23% had nonischemic findings, the most common of which were myocarditis and nonischemic cardiomyopathy, she said.
There was no difference by sex in ischemic findings on MRI (women, 42%; men, 30%; P = .12) or in nonischemic findings on MRI (women, 23%; men, 25%; P = .78), the researchers found.
Independent predictors of an abnormal cardiac MRI were higher peak troponin, non-Asian race and shorter time between MI and cardiac MRI, Reynolds said.
Among the patients who had both OCT and cardiac MRI, 79% had a cause identified (MI, 59%; a MINOCA mimic, 20%) and 21% did not, she said, noting that combining modalities was more likely to identify a cause than OCT alone (44%) or cardiac MRI alone (69%; P < .001 for both).
“We found things that significantly predicted the likelihood of a culprit lesion or of having abnormal cardiac MRI, but they weren’t overpowering,” Reynolds told Healio. “It’s a lesson that you just have to do the imaging if you want to find the underlying cause. I hope that this will lead to earlier application of cardiac MRI and more consistent application of cardiac MRI.”
DISCOVER-INOCA
DISCOVER-INOCA was a prospective multicenter registry of 500 patients (mean age, 57 years; 78% women) undergoing invasive coronary function testing. All patients had suspected ischemic heart disease but no obstructive CAD and none had MI at presentation or within 90 days before.
The primary short-term endpoint was prevalence of each INOCA physiologic phenotype, as defined by the COVADIS criteria, after coronary function testing, and the secondary endpoint was major adverse CV events, defined as CV death, MI, hospitalization for CV cause or coronary revascularization, at 30 days, Samit Shah, MD, PhD, interventional cardiologist and assistant professor of medicine at Yale School of Medicine, said during a presentation.
More than 99% of patients completed physiologic testing (acetylcholine provocation, fractional flow reserve and/or coronary flow reserve) and more than 96% completed intravascular imaging, he said.
Among the cohort, 94% had a diagnosis of a coronary vasomotor disorder (vasospastic angina, 36%; coronary microvascular dysfunction, 16.8%; mixed vasospastic angina/ coronary microvascular dysfunction, 27.8%; other disorders, 13.8%), 89% had a change from their preprocedural empiric diagnosis and 72% had their medication changed after their procedures, Shah said during the presentation.
At 30 days, Seattle Angina Questionnaire summary score improved in patients with vasospastic angina (P < .001), mixed vasospastic angina/coronary microvascular dysfunction (P = .008) and other coronary vasomotor disorders (P < .001), he said.
The rate of procedural serious adverse events was 1.4%, he said.
Major adverse CV events occurred in 1.8% of patients at 30 days, with 0.7% having MI and 1.2% being hospitalized for a CV cause, Shah said.
“Coronary function testing had a favorable safety profile with a low but nontrivial rate of procedure-related serious adverse events,” he said during the presentation. “These findings support routine use of comprehensive invasive coronary function testing to identify vasomotor disorders and guide medical therapy in patients with INOCA.”
For more information:
Harmony R. Reynolds, MD, can be reached at cardiology@healio.com.
<












Leave a Reply