April 15, 2026
1 min read
Key takeaways:
- Adolescents wearing ortho-K lenses had significantly lower tear film instability and greater meibomian gland loss.
- Regular follow-up and close monitoring of ocular surface health are needed.
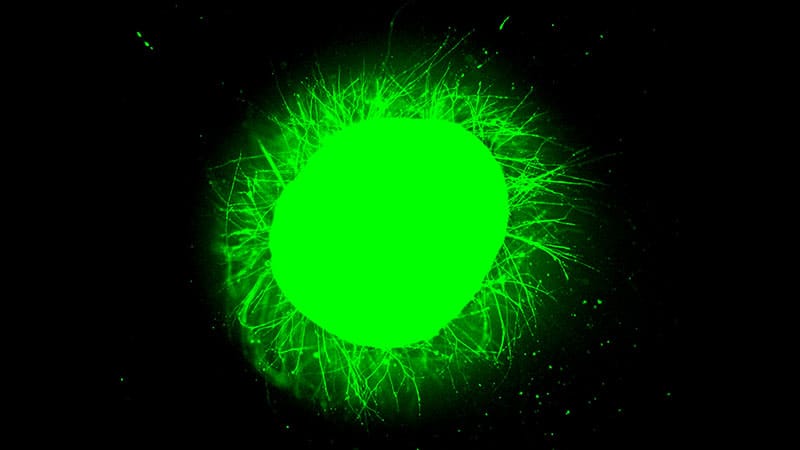
Wearing orthokeratology lenses to control myopia progression may pose risks to ocular surface health, including loss of meibomian glands and tear film instability, according to a study published in Contact Lens & Anterior Eye.
“Contact lenses have several advantages, but they act as foreign bodies on the eye and can alter the normal structure of the tear film,” Xiao-Di Yang, of First Affiliated Hospital of Zhengzhou University, China, and colleagues wrote. “[Orthokeratology] lenses are corneal contact lenses worn overnight. … Several studies have examined their effects on the ocular surface. However, the longest follow-up duration reported by these studies was 2 to 3 years.”

Wearing orthokeratology lenses to control myopia progression may pose risks to ocular surface health, including loss of meibomian glands and tear film instability. Image: Adobe Stock
Yang and colleagues conducted a cross-sectional study of 60 adolescents, 30 of whom had worn orthokeratology lenses for at least 5 years (mean duration, 5.75 years) and 30 of whom wore spectacles. They matched the patients demographically and compared visual acuity, meibomian gland loss, corneal fluorescein staining, tear meniscus height and noninvasive tear breakup time.
According to the results, orthokeratology wearers had significantly lower tear film stability and greater loss of meibomian glands in the lower eyelid compared with non-wearers.
The loss of meibomian glands in the lower lid increased by 4.044% for each 1 D reduction in myopia. Losses were greater in boys than girls after adjusting for other factors (P = .003).
Wearers of orthokeratology lenses also had significantly thinner tear film lipid layers (P = .008) and lower noninvasive tear breakup time (P = .04) on average, further indications of compromised ocular surface health.
Yang and colleagues noted that while none of the orthokeratology wearers experienced “marked ocular discomfort,” the results still show that “the degree of [orthokeratology] correction is a factor affecting the safety of wear.”
“The specific reasons and mechanisms require further investigation,” they wrote. “These findings highlight the importance of regular follow-up during lens wear. They also emphasize the need for wearers of [orthokeratology] lenses and ophthalmologists to monitor ocular surface health closely.”
<














Leave a Reply