April 15, 2026
2 min read
Key takeaways:
- Adults with low-risk thyroid cancer had similar patient-reported outcomes, regardless of treatment choice.
- Patients who switched from active surveillance to surgery had increased cancer worry.
Most patient-reported outcomes for patients with low-risk thyroid cancer who underwent active surveillance are similar to those who opted for surgery, according to findings published in Thyroid.
As Healio previously reported, adults diagnosed with low-risk papillary thyroid cancer at a University Health Network clinic in Toronto had low levels of treatment decision regret at 1 year, regardless of whether they selected active surveillance or surgery. In new data published from the same health system, researchers found few differences in patient-reported outcomes between the active surveillance and surgical groups, though a small group of adults who switched from active surveillance to surgery reported greater levels of cancer worry and treatment decision regret.

Data were derived from Sawka AM, et al. Thyroid. 2026;doi:10.1177/10507256251408857.
“It is well known that many patients prioritize quality of life in considering low-risk papillary thyroid carcinoma disease management options,” Anna M. Sawka, MD, PhD, endocrinologist and clinician scientist at University Health Network and University of Toronto, told Healio. “Our findings suggest that for well-informed patients with small, low-risk papillary thyroid carcinoma evaluated a few years after deciding on active surveillance or surgery, quality of life may not significantly differ according to the treatment choice.”

Anna M. Sawka
Sawka and colleagues conducted a prospective cohort study of adults aged at least 18 years diagnosed with papillary thyroid cancer with a tumor less than 2 cm in diameter. Adults who chose active surveillance attended a follow-up every 6 months for 2 years, followed by annually thereafter. Patients who initially chose active surveillance could undergo surgery at any point.
There were 120 patients in the study, of whom 98 initially chose active surveillance and 22 underwent surgery immediately after diagnosis (median age, 53 years; 74% women). Of adults in the active surveillance group, 16 later underwent surgery, with eight having surgery following disease progression, seven opting for surgery by choice and one patient having surgery due to uncertainty in tumor measurement.
Adults who chose active surveillance had similar patient-reported outcome scores as those who underwent surgery in all questionnaires.
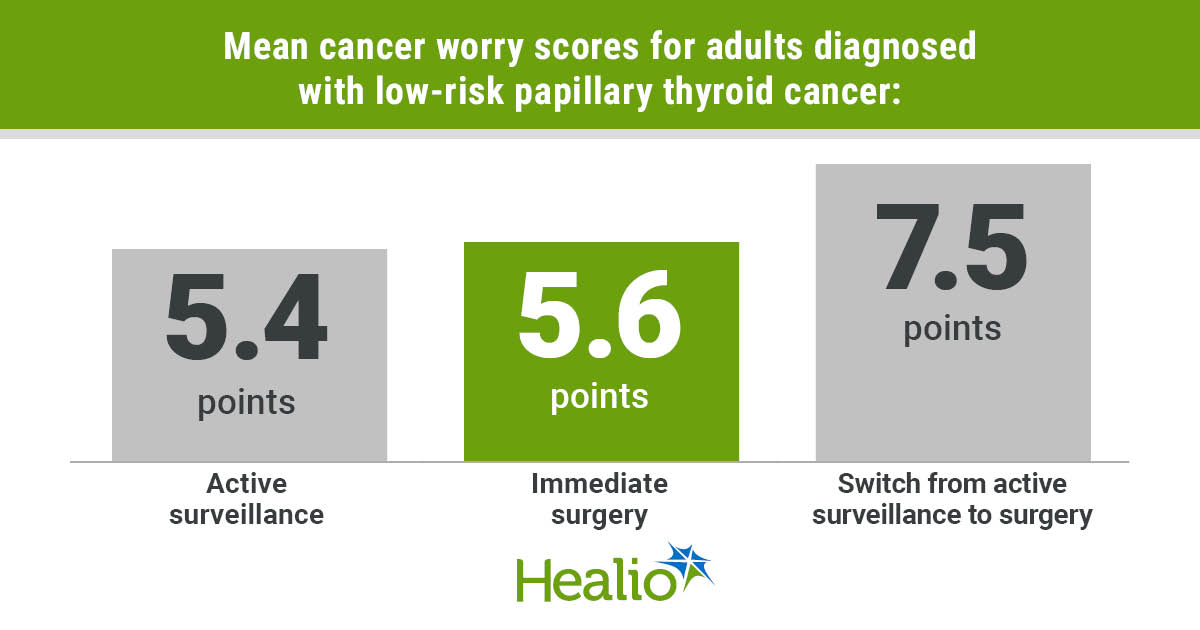
On the Assessment of Survivor Concerns questionnaire, adults who switched from active surveillance to surgery had higher cancer worry scores (mean score, 7.5 points) vs. those who underwent surgery at baseline (mean score, 5.6 points) and those who remained in active surveillance (mean score, 5.4 points; P = .021). Similarly, overall worry summary score on the questionnaire was higher for those changing from active surveillance to surgery than the other two groups (P = .021).
Sawka said the increased worry for patients who switched treatment options was not surprising, noting that some patients had cancer progression that may have increased worry, whereas others may have changed their mind due to continued cancer concerns, even in the absence of progression.
“It will be important to continue to follow the patients who crossed over with longer-term follow-up to ascertain whether their level of worry and decision regret improve over time,” Sawka said.
Adults who switched from active surveillance to surgery reported feeling a greater level regret about their treatment decision (mean score, 27.2 points) than those who had surgery at diagnosis (mean score, 21.1 points) and adults who remained in active surveillance (mean score, 17.9 points; P = .031). In post hoc exploratory analysis, seven adults who chose to switch from active surveillance to surgery without disease progression had higher decision regret scores than the eight adults who switched to surgery due to cancer progression (38.9 points vs. 19 points). Other patient-reported outcomes did not differ between those two groups.
Sawka said large, prospective studies need to be conducted to confirm the findings.
For more information:
Anna M. Sawka, MD, PhD, can be reached at endocrinology@healio.com.
<












Leave a Reply