Key takeaways:
- Non-tobacco nicotine use raised the risk for over a dozen adverse outcomes, including death and cesarean birth.
- The data show a need for greater screening and education on nicotine use, researchers said.
WASHINGTON — Non-tobacco nicotine use before a positive pregnancy result increased the risk for pregnancy and delivery complications, according to research at the ACOG Annual Clinical & Scientific Meeting.
Madeline West, the study’s lead author from the Paul L. Foster School of Medicine at Texas Tech Health Sciences Center El Paso, told Healio that the analysis “was driven by the increasing use of non-tobacco nicotine products — especially vaping and e-cigarettes — among reproductive-age patients. While the risks of traditional cigarette smoking during pregnancy are well established, many patients perceive vaping as a safer alternative. At the same time, there is far less pregnancy-specific data on these newer nicotine products.”

Data derived from West M, et al. Non-tobacco nicotine products and their association with adverse pregnancy outcomes: A multi-institutional 1:1 propensity matched cohort analysis. Presented at: ACOG Annual Clinical & Scientific Meeting; May 1-3, 2026; Washington.
“Given our focus in obstetrics and women’s health, we wanted to better understand whether these exposures are associated with adverse pregnancy outcomes and whether they should be approached with the same level of concern as traditional tobacco use,” she said.
In the study, West and colleagues assessed the effects of non-tobacco nicotine dependence (NTND) on labor, maternal and fetal outcomes among 77,549 patients from the TriNetX database. The participants were propensity score matched 1:1.
The researchers reported that NTND was associated with higher risks for:
- preterm labor (RR = 1.717);
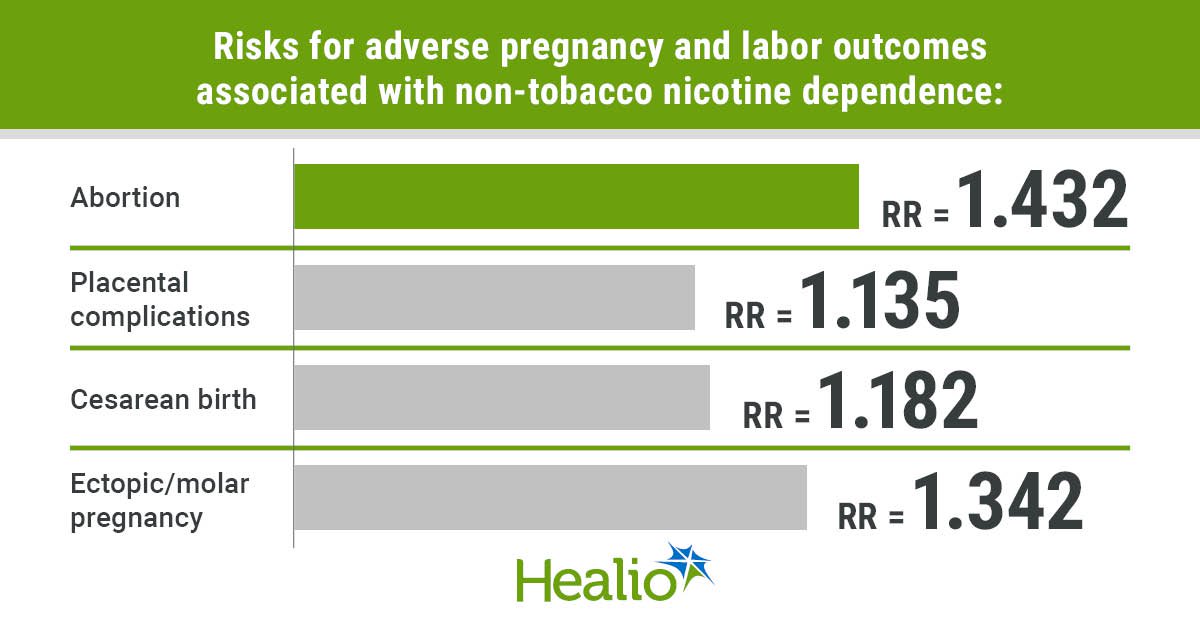
- abortion (RR = 1.432);
- ectopic/molar pregnancy (RR = 1.342);
- placental complications (RR = 1.135); and
- cesarean birth (RR = 1.182).
Several serious complications, including myocardial infarction (RR = 2.422), death (RR = 2.522), deep vein thrombosis (RR = 1.445), infection (RR = 1.445), wound complications (RR = 1.941) and pulmonary embolism (RR = 1.691), were also more common among patients with NTND.
West and colleagues additionally found NTND was associated with greater ED visits (RR = 1.416), opioid abuse (RR = 15.743) and readmissions (RR = 1.466).
NTND was not tied to sepsis; hemolysis, elevated liver enzymes and low platelets syndrome; hemorrhage; or congenital cardiac anomalies.
West said the findings underline “an important clinical message: ‘safer’ does not mean safe, especially during pregnancy. Just because a product does not contain combustible tobacco does not mean it is harmless. Nicotine itself has significant physiologic effects that can impact both maternal and fetal health.”
She noted that a “striking” finding was the strong link between NTND and opioid abuse. “This does not imply causation, but it highlights that nicotine exposure may serve as an important marker for broader high-risk health behaviors and social factors that require closer attention during prenatal care,” she said.
Health care professionals “should broaden how they screen for nicotine use in pregnancy,” West explained. “Many patients do not consider vaping, nicotine pouches, or other non-tobacco nicotine products to be ‘tobacco use,’ so these exposures may go unrecognized unless we ask specifically.”
Clinician counseling on non-tobacco nicotine use “should reflect that nicotine itself — not just cigarettes — can contribute to adverse pregnancy outcomes. As nicotine use evolves, our screening and patient education need to evolve as well,” West said.
Nicholas Stansbury, MD, FACOG, a study co-author and specialist fellow at the University of Texas Health San Antonio, told Healio that additional prospective research on the effects of non-tobacco products is necessary, “particularly as these products become more common. Larger studies and future systematic reviews will help clarify the true magnitude of risk and whether certain products may be more harmful than others. We also need better patient education and cessation strategies specifically designed for vaping and alternative nicotine products, since many current counseling approaches are still focused primarily on traditional cigarette smoking.”
Ultimately, the greatest takeaway from the data “is that the conversation around nicotine use in pregnancy has changed,” Stansbury said. “We can no longer focus only on cigarettes. Patients are increasingly using newer nicotine products with the belief that they are safer or harmless. Our responsibility as physicians is to make sure our counseling reflects the current evidence and addresses all forms of nicotine exposure.”
For more information:
Madeline West and Nicholas Stansbury, MD, FACOG, can be reached at primarycare@healio.com.
<













Leave a Reply